Review highlights progress toward imaging strategies that dynamically measure how the spine functions
Low back pain affects hundreds of millions of people worldwide, often striking during everyday movements. In most cases, standard imaging techniques, which provide snapshots of the spine’s anatomy, cannot pinpoint the cause.
“Pain doesn’t always show up when you’re lying still,” said Dawn Elliott, Blue and Gold Distinguished Professor of Biomedical Engineering at the University of Delaware. “It can happen when you’re standing or bending or under certain loads. Just taking a picture without any of that context isn’t enough.”
Everyone’s spine is different, and normal aging can look like disease on routine scans—spinal discs naturally lose water and begin to degenerate over time. Pain often depends on how the spine behaves under movement, posture and load.
To address this, researchers are developing advanced noninvasive imaging methods that focus on spinal function, not just structure. A new invited review by Elliott and colleagues, appearing in npj Biomedical Innovations, explores how different techniques can be harnessed to capture these mechanical insights.
Each imaging modality has its own strengths and limitations. X-rays are effective for visualizing bone but cannot capture soft tissues like muscles and discs. Ultrasound is portable and can track real-time movement as a person bends or stretches, but it produces lower-resolution, two-dimensional images. Magnetic resonance imaging (MRI) yields high-resolution, three-dimensional data that can offer rich mechanical insights. However, it requires patients to remain still during imaging, limiting the range of motion that can be studied.
“There’s a time and place for all of these,” Elliott said. “But we think MRI offers more opportunities than the others, and that is the area in which we focus.”
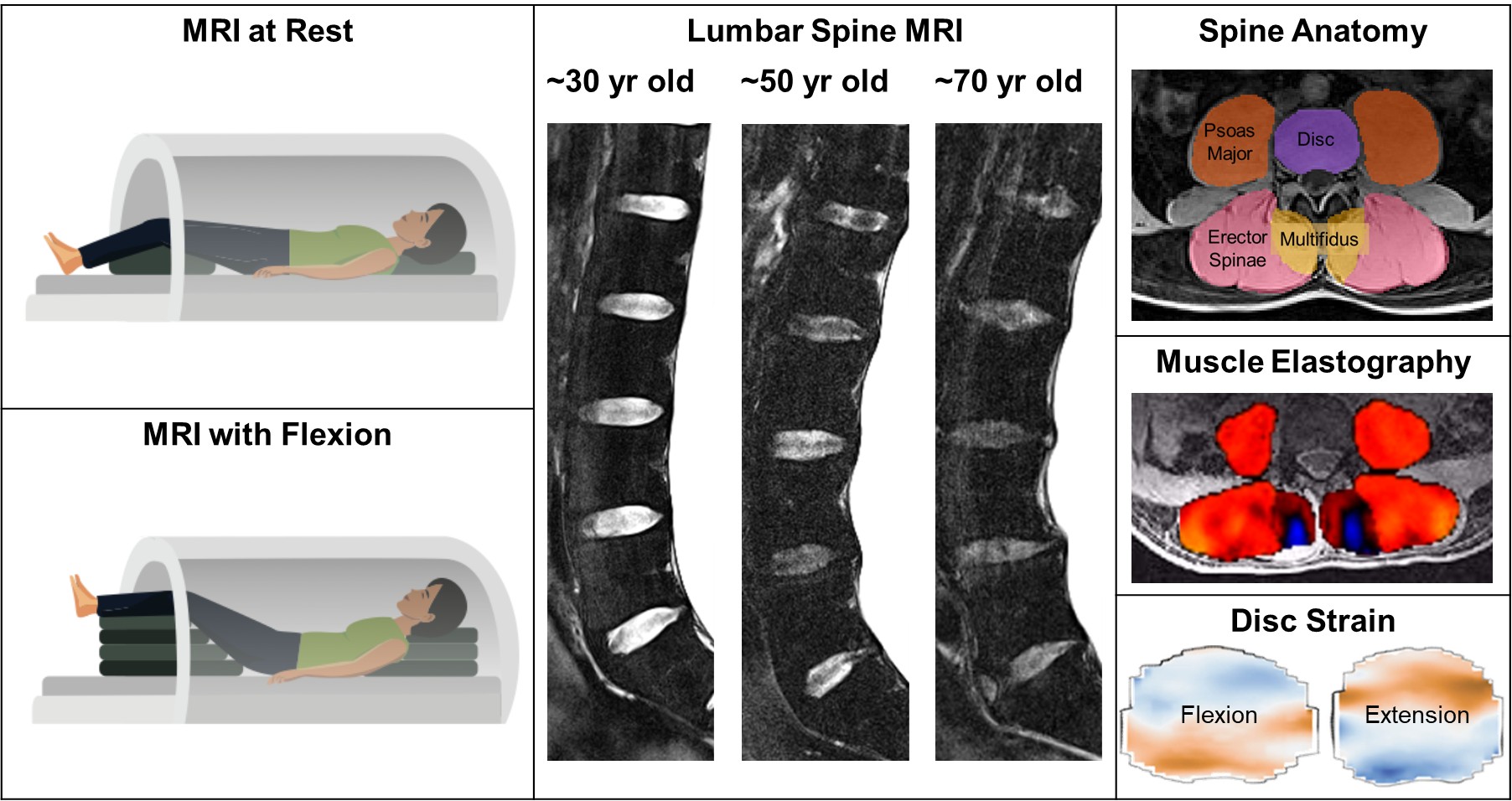
Left: Position in MRI at rest and in flexion. Middle: Sagittal MRI view of lumbar spine with normal age-related disc degeneration (discs are darker and shorter) with no back pain. Right: Axial MRI view showing disc and spine muscle anatomy, muscle elastography and disc strain in flexion and extension postures.
Researchers are working to develop faster, more automated ways to translate MRI data into measures of tissue mechanics, often combining imaging with computational models to estimate forces and pressures within the spine. Advances in artificial intelligence may help accelerate that process by integrating complex imaging data with patient-specific information.
Distinguishing aging from disease remains a key challenge. To address this, Elliott’s team recently developed a method to quantify expected aging-related changes in spinal discs, providing researchers a tool to help identify when degeneration may be linked to pain.
Efforts also are underway to apply MR elastography, a technique that measures tissue stiffness to better understand how muscles function, to study back pain.
“Muscle is doing mechanical work, and its mechanics are closely tied to its function,” said review co-author Curtis Johnson. “If you flex a muscle, it gets stiffer. We can measure those changes and begin to estimate how much force it’s producing and what it’s capable of.”
Elliott estimates it could take five to 10 years for advanced MRI techniques for low back pain to reach clinical use. In the meantime, the work is already helping scientists better understand the underlying causes of such pain. Ultimately, the goal is to move beyond static snapshots toward a more complete picture of spinal health that captures not just what the spine looks like, but how it works.
Other co-authors of the review are UD postdoctoral researcher Harrah Newman, UD doctoral student Mackenzie Conner and orthopedic surgeon Edward Vresilovic.
Article by Hillary Hoffman | Image provided by Dawn Elliott & Pixabay

